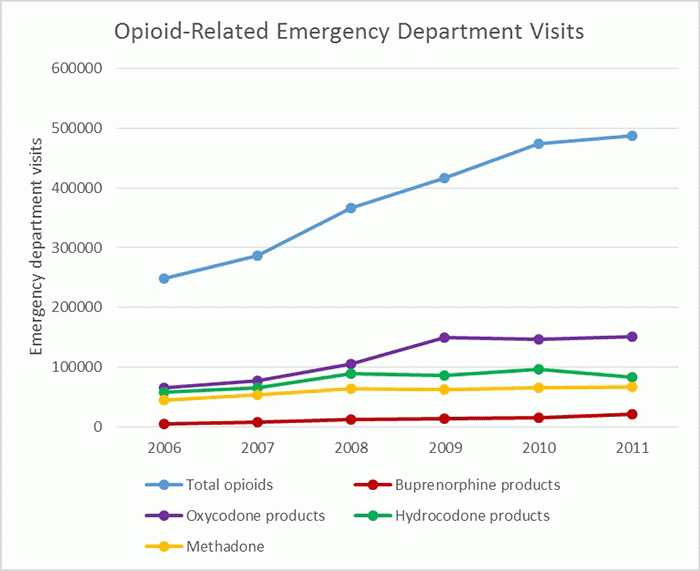
Like other opioid medications, buprenorphine and methadone are sometimes diverted and misused. However, most data suggest that the majority of buprenorphine and methadone misuse (use without a prescription) is for the purpose of controlling withdrawal and cravings for other opioids and not to get high. Among all opioid agonist medications, methadone and buprenorphine together make up 15 percent of diversion reports, while oxycodone and hydrocodone are responsible for 67 percent.43 Naltrexone, an opioid antagonist used to treat opioid addiction, does not cause euphoric effects and is not a diversion risk.
Diversion Risk of Buprenorphine
Both buprenorphine and buprenorphine/naloxone formulations can interfere with the effects of full opioid agonists, such as heroin, and can precipitate withdrawal in individuals with opioid dependence. Two U.S. surveys of people with opioid use disorder found that a majority of those who used illicit buprenorphine reported that they used it for therapeutic purposes (i.e., to reduce withdrawal symptoms, reduce heroin use, etc.).44,45 Ninety-seven percent reported using it to prevent cravings, 90 percent to prevent withdrawal, and 29 percent to save money.45 Illicit use of buprenorphine decreased as individuals had access to treatment.45 The minority proportion of people who use buprenorphine illicitly to get high (ranging from 8 to 25 percent)45,46 has been shown to decrease over time, which could suggest that people abandon this goal after they experience the drug’s blunted rewarding effects.46 Indeed, patients in treatment for opioid use disorder rarely endorse buprenorphine as the primary drug of misuse.47
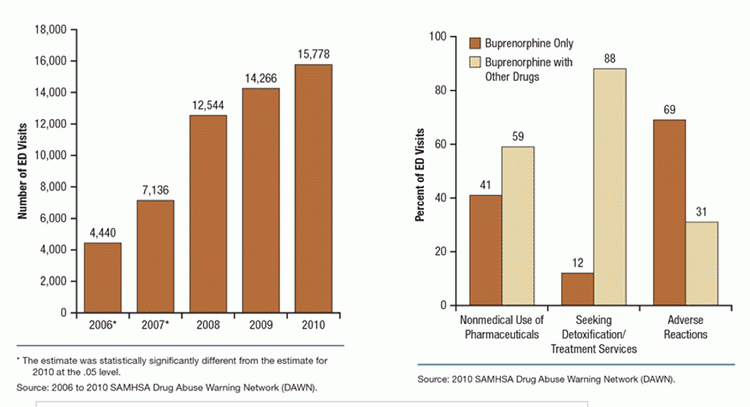
While there is some risk associated with misuse of buprenorphine, the risk of harms, such as fatal overdose, are significantly lower than those of full agonist opioids (oxycodone, hydrocodone, heroin).39,51 Overdoses and related deaths do occur but are usually the result of combination with other respiratory depressant drugs such as benzodiazepines or alcohol. Emergency department (ED) visits involving buprenorphine increased from 3,161 in 2005 to 30,135 visits in 2010 as availability of the drug increased (buprenorphine was first approved in 2002); but ED visits for buprenorphine remain significantly less common than those for other opioids.52 Fifty-two percent, or 15,778 visits (see left bar chart below), were related to nonmedical use in 2010; 59 percent of these visits involved additional drugs (see right bar chart below).53,54
Diversion Risk of Methadone
Methadone diversion is primarily associated with methadone prescribed for the treatment of pain and not for the treatment of opioid use disorders. Opioid treatment programs are required to maintain and implement a diversion control plan; they typically require patients to come in daily to receive their medication and strictly monitor take-home doses. In addition, evidence suggests that the diversion that does occur is associated with a lack of access to medication.48 In one survey, giving methadone away was identified as the most common form of methadone diversion,49 which aligns with other findings that 80 percent of people who report diverting methadone did so to help others who misused substances.48,50 Among those using illicit methadone, the most common reason was a missed medication pick-up.50
Methadone, as a full opioid agonist that is metabolized slowly, poses a greater risk of overdose than buprenorphine. In 2010, 65,945 ED visits involved nonmedical use of methadone.53 However, methadone that is dispensed for use as a pain reliever, not as an substance use disorder medication, is the main source of the methadone involved in overdose deaths.55