This study:
- Demonstrated that functional connectivity among a large number of brain regions predicts patients' chances of achieving abstinence in treatment for cocaine use disorder.
- Raised the prospect that altering connectivity among the regions might be an effective way to treat the disorder.
NIDA-supported scientists have shown how to use functional magnetic resonance imaging (fMRI) and machine learning to predict patients' outcomes in treatment for cocaine use disorder. Their findings have promising implications for both research and treatment.
Dr. Sarah W. Yip and colleagues at Yale University recruited 53 men and women who had volunteered to participate in a clinical trial of the medication galantamine. At the start of the trial, the researchers performed whole-brain fMRIs while the patients played a reward game ("Monetary Incentive Delay Task") that activates regions of the brain known to be implicated in drug use. The patients then received 12 weeks of behavioral therapy, with or without galantamine. They provided biweekly urine samples to test for cocaine throughout the treatment.
The researchers fed the fMRI and drug use data into a machine-learning algorithm for analysis. (See the textbox for more information on machine learning.) The machine-learning algorithm they used is a recently developed approach designed for neuroimaging data, called connectome-based predictive modeling. The algorithm revealed significant correlations between connectivity (coordinated responses) in 529 neuronal pathways and patients' cocaine use during treatment. Treatment success was correlated with stronger connectivity in about half the pathways and with weaker connectivity in the others.
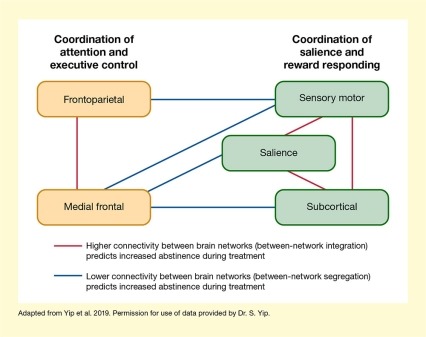
The 529 pathways linked a large number of distributed brain regions. To summarize the overall pattern of connections, the researchers proposed a five-network model that relates their findings to commonly studied, well-established brain networks. Strong connectivity between two networks (frontoparietal and medial frontal) that serve executive control functions correlated with abstinence. So did strong connectivity among three other networks (salience, sensory motor, and subcortical) that regulate responses to rewards. However, strong connectivity in pathways that joined the executive pair to the reward responsiveness trio was associated with reduced likelihood of abstinence (see Figure).
Prediction scores
Dr. Yip and colleagues demonstrated that the functional connectivity within the networks identified by the machine-learning algorithm could be used to predict individual patients' success or failure in treatment. The researchers confirmed the procedure by showing that prediction scores generated from the same networks of patients in another, unrelated treatment study also distinguished those who achieved abstinence from those who did not. For each patient in the separate study, they recorded the connectivity strength of each of the 529 connections from the patient's fMRI and then summed them all to create an abstinence prediction score. When they then correlated these scores with the patients' actual abstinence values, they found a significant association, indicating a high predictive accuracy.
Dr. Yip says, "These data demonstrate, for the first time, that individual differences in substance use outcomes can be predicted from whole-brain patterns of functional connectivity in a data-driven manner. This is a critical step toward the development of reliable, brain-based markers of treatment outcomes."
The researchers showed that prediction scores based on connectivity are stable and have long-term predictive value. They examined 40 patients who were scanned before and after treatment and found that their scores had not changed with treatment. Moreover, the scores predicted which patients were abstinent and which were not at follow-up testing 6 months after treatment.
Dr. Yip says, "Unlike traditional statistical approaches, machine-learning methods are designed to generate predictions in novel data. They therefore have tremendous potential to inform clinical decision-making through individual prediction of outcomes." One potential use of the method would be to balance patients in the treatment and control groups of a clinical trial with respect to their potential to benefit from treatment. Dr. Yip and colleagues found that the prediction scores based on connectivity predicted their patients' treatment outcomes better than the clinical and demographic characteristics that researchers currently use for such balancing. More exciting, connectivity relationships may provide clues for the development of effective new treatments. For example, treatments might be tailored to alter connectivity in ways that increase patients' abstinence prediction scores.
Machine Learning
Machine learning, a branch of artificial intelligence, is a computer-based approach of data analysis using programs and algorithms that allow the computer to automatically "learn" without being explicitly programmed. The computer is initially trained to recognize certain patterns in data using a set of known training data (e.g., from known examples or tests). The computer can then apply this information to new data to identify new patterns and make inferences, predictions, or decisions without additional input from programmers. Machine learning allows for the faster and more accurate analysis of massive amounts of data and information than would otherwise be possible, such as those necessary for tasks as diverse as self-driving cars, speech recognition, and analysis of the human genome.This study was supported by NIDA grants DA039299, DA009241, and DA035058.
- Text Description of Figure
-
The figure illustrates how connectivity between five brain networks influences abstinence during treatment for cocaine use disorder. Five rectangles indicate the five brain networks. The two orange rectangles on the left represent networks related to coordination of attention and executive control: The frontoparietal network (top) and the medial frontal network (bottom). The three green rectangles on the right represent three networks related to coordination of salience and reward responding: the sensory motor (top), salience (middle), and subcortical (bottom) networks. Red lines between the frontoparietal and medial frontal networks, as well as salience and sensory motor, salience and subcortical, and sensory motor and subcortical networks indicate that higher connectivity between these networks, also known as between-network integration, predicts increased abstinence during treatment. Blue lines between the frontoparietal and sensory motor, medial frontal and sensory motor, medial frontal and salience, and medial frontal and subcortical networks indicate that lower connectivity between these networks, also known as between-network segregation, predicts increased abstinence during treatment.
Source:
- Yip, S.W., Scheinost, D., Potenza, M.N., Carroll, K.M. Connectome-based prediction of cocaine abstinence. American Journal of Psychiatry 76(2):156-164, 2019.